
|
|
Research HighlightResearch Points to Importance of VA and Community Care Patient Experience ScoresThrough the Choice Act of 2014 and the MISSION Act of 2018, VA has vastly increased the amount of healthcare it purchases in the community for its enrolled Veterans. Improving access to timely, high-quality care was the primary intent of both these Acts. Measuring access to and the quality of VA and community care is difficult since comparisons must account for patient-level and system-level factors that could affect the outcomes. Nonetheless, comparisons between VA and community care remain a high priority for VA leaders and policy makers, such as VA’s Office of Reporting, Analytics, Performance, Improvement and Deployment and VA’s Office of Community Care. Our recent study, published in the August issue of Health Affairs,1 used data from the Survey of Healthcare Experiences of Patients (SHEP) to compare the outpatient experiences of Veterans who received VA-delivered care with those who received VA-purchased care. Outpatient SHEP questions are based on the industry standard for patient experience, the Agency for Healthcare Research and Quality’s Consumer Assessment of Healthcare Providers and Systems Clinician & Group Survey (CG-CAHPS). We examined Veterans’ perceptions of access, coordination, communication, and provider rating separately for primary care, mental health care, and other specialty care by quarters from Federal Fiscal Year 2016 quarter 2 through 2017 quarter 4. Veterans’ self-reported experiences of care are increasingly considered key outcome measures as VA focuses on becoming a Veteran-centered learning health system. They are also fundamental to measuring access and quality. We found that VA outperformed community care on all SHEP measures except access, in which the community scored better on specialty care access; no differences were found for primary or mental health care access by site of care (see Figure below). In some cases, baseline VA scores were considerably higher than those in the community (e.g., primary care coordination, where a 15 percent difference was found). In other cases, VA and community care scores were not meaningfully different at baseline (e.g., specialty care provider rating, where a 2 percent difference was found). Although some patient experience scores increased over time (specifically, primary care coordination and all four specialty care scores), the gap between VA and community care scores did not decrease over time. In summary, while Choice improved access to care, patient experience appears to be quite similar between VA and community care in some cases, and markedly better at VA in others. Findings such as these point to the importance of incorporating Veteran perceptions of care in the monitoring of patient care and policy impact over time. Quality of care comparisons are now required by the MISSION Act. VA has developed a MISSION Act Quality Standards Tracking Report (MAQSTR), but metric scoring had to besuspended through Fiscal Year 2020 because of disruption of measure collection due to COVID-19. In addition to its utility for VA and community care comparisons, MAQSTR presents researchers with opportunities to compare patient experiences across other federal payers, including the Department of Defense (DoD) and Health and Human Services (HHS). Since the outpatient SHEP questions are based on CG- CAHPS, it would also be possible to use these measures in order to harmonize data across federal systems through HHS’ Quality Roadmap. The Roadmap is part of Executive Order 13877, Improving Price and Quality Transparency in American Healthcare to Put Patients First, which was released on May 15, 2020. In summary, there is much promise for patient experience data to be used for comparisons of access and quality both within VA and for VA to community care comparisons, as well as across other payer and provider systems funded by the federal government. 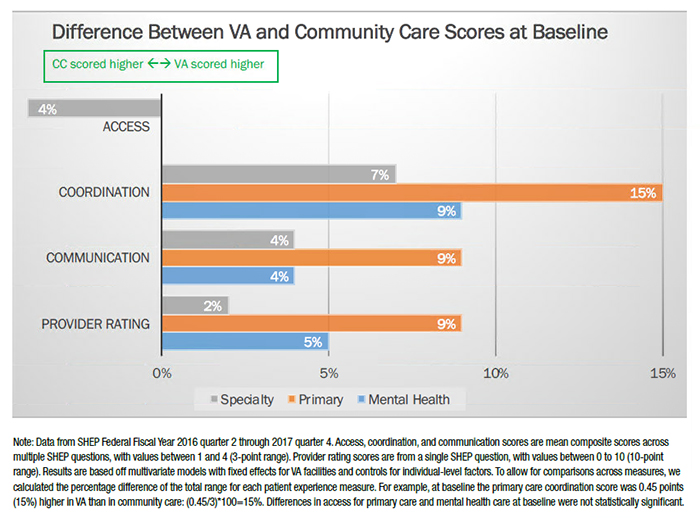
References
|
|