|
The report is a product of the VA/HSR Evidence Synthesis Program.
Evidence Map: Women Veterans' Health Research Literature (2008-2015)
As the number of women who serve in the military continues to increase, the provision of high-quality, evidence-based, accessible healthcare for women Veterans has become a vital strategic priority within VA. A growing body of literature addresses the health and healthcare concerns of women Veterans. The VA Women's Health Research Network, established in 2010, seeks to systematically improve women's healthcare and reduce sex/gender disparities by filling critical knowledge gaps in the evidence base related to women Veterans' health and healthcare needs.
To help address these gaps in the evidence, investigators with VA's Evidence-based Synthesis Program Center located in Minneapolis, Minnesota conducted a literature search (MEDLINE, CINAHL, and HSR&D database) for articles published between 2008 and 2015 on women Veterans' health research. After reviewing 2,276 abstracts, investigators included 437 references to create an evidence map around healthcare topics of interest according to key study characteristics in order to facilitate planning of future VA research, policy, and clinical activities in women Veterans' health. Investigators included all interventions, comparators, outcomes, and settings. Due to the breadth of research included, they did not extract, evaluate, or present study findings.
Summary of Review
A large and varied body of research represents a growing evidence base that can be leveraged to improve the health of women Veterans. Significant progress has been made toward achieving the ambitious research agenda set forth during the 2010 VA Women's Health Services Research Conference; however, investigators identified several persistent gaps in the literature.
Key findings include:
- Nearly half (47%) of the included studies were related to mental health. Other specific health conditions or categories accounted for fewer than 10% of studies.
- More than 90% of studies were observational; investigators identified only 8 (2%) randomized controlled trials or controlled clinical trials and 12 (3%) secondary analyses of trials.
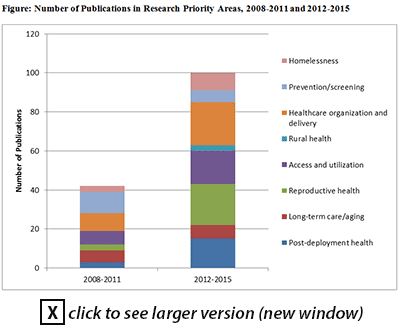
- Of six key topic areas established at the 2010 VA Women's Health Services Research Conference, dramatic growth in the number of publications – and to some extent advances beyond observational research – were noted for four areas:
- Access to care and rural health,
- Post-deployment health,
- Reproductive health, and
- Mental health.
- Two key areas did not increase much in publications: 1) primary care and prevention (except for a subtopic area – organization and delivery of primary and comprehensive care for women Veterans), and 2) complex chronic conditions/long-term care and aging.
VA research and clinical stakeholders can use the evidence map included in this report to help direct the future of women Veterans health research.
Future Research
Capturing Ongoing Research
One of the initial limitations in developing this literature map was the large quantity of published articles that included women Veterans, but provided results only for the complete study population and not for the sub-population of women Veterans. In this situation, study results cannot be directly interpreted and applied by women Veterans' providers and researchers. The need for sex-specific reporting of scientific research results has been recognized by both the National Institutes of Health and the Institute of Medicine. Research related to Veterans, which often utilizes the national VA administrative databases, may be more likely to have the statistical power to report subgroup analysis results by sex or gender than non-VA health research. Additionally, as a source of research funding the VA may be positioned to require the inclusion of specific results-reporting for women in research studies. Women Veterans' health stakeholders should champion efforts to capitalize on the large body of research in which women Veterans are already participating.
Social and Cultural Transitions
Social and cultural shifts within both the U.S. military and American society also will provide opportunities for expanded research related to women Veterans health. Examples include experiences of LGBT Veterans following the end of the "Don't Ask, Don't Tell" policy (2011), and the more recent move to allow openly transgender service members (2016). In addition, the expanding role of women in combat following the lifting of the Combat Exclusion Policy (2013) may have significant implications for research related specifically to women with traumatic brain injury, spinal cord injury, and amputations. Increased combat exposure also may result in changes in PTSD among women Veterans. Finally, a transition in the national discussion of sexual assault may filter into future research and policy related to Military Sexual Trauma, which has affected many women Veterans.
Veteran Engagement
VA is increasingly seeking to engage Veterans in research by including Veteran stakeholder perspectives in research processes such as development of study questions, selection of outcome measures, and interpretation of findings. None of the included studies described Veteran engagement as a component of their methods, although several studies incorporated Veterans' perspectives (e.g., qualitative input to improve an intervention). Thus engagement with women Veterans as research stakeholders or partners is an important potential area for future research innovation.
A Cyberseminar session will be held to discuss this ESP report on Monday, February 13, 2017 from 1:00pm to 2:00pm (ET). To register, go to the HSR&D Cyberseminar web page.
Reference
Danan E, Ensrud K, Krebs E, Koeller E, Greer N, Velasquez T, MacDonald R, Wilt, TJ. An Evidence Map of the Women Veterans' Health Research Literature (2008 – 2015). VA ESP Project #09-009; 2016.
View the full report — **VA Intranet only**:
http://vaww.hsrd.research.va.gov/publications/esp/womens-health2.cfm
(copy and paste if you have VA intranet access)
|
Please feel free to forward this information to others!
Read past HSR&D Management e-Briefs on the HSR&D website.
ESP is currently soliciting review topics from the broader VA community. Nominations will be accepted electronically using the online Topic Submission Form. If your topic is selected for a synthesis, you will be contacted by an ESP Center to refine the questions and determine a timeline for the report.
This Management e-Brief is provided to inform you about recent HSR&D findings that may be of
interest. The views expressed in this article are those of the authors and do not necessarily
reflect the position or policy of the Department of Veterans Affairs. If you have any questions or
comments about this Brief, please email CIDER.
The Center for Information Dissemination and Education Resources (CIDER) is a VA HSR&D Resource
Center charged with disseminating important HSR&D findings and information to policy makers, managers,
clinicians, and researchers working to improve the health and care of Veterans.
|
