» Back to list of all Management Briefs

| Issue 161 | November 2019 | |
|
The report is a product of the VA/HSR Evidence Synthesis Program. Effectiveness of Remote Triage: Systematic ReviewThe US healthcare system currently faces several challenges including caring for an increasing elderly population, an increasing patient population with multiple chronic conditions, and an uneven distribution of primary care providers. Additionally, many patients experience multiple barriers to receiving timely care, such as financial and logistical impediments. Such access challenges lead many people to seek acute or chronic care in emergency departments (EDs) when their needs might have been addressed in a primary care setting. Increasingly, acute care visits take place outside of the primary care setting. One way of providing patient access to the appropriate level of care is through technology-based systems that facilitate remote decision-making about healthcare.
VA's Evidence Synthesis Program (ESP) Center in Durham, NC examined the impact of remote triage on outcomes that were meaningful to VA operations stakeholders (i.e., VA's Office of Connected Care), clinicians, and policymakers and explored emerging practices for implementing a remote triage system. Investigators searched MEDLINE (via PubMed), EMBASE, and CINAHL from inception through July 27, 2018; they also examined bibliographies of recent reviews for additional relevant studies. The literature search identified 11,939 relevant articles. Of these, 9 were identified as relevant studies assessing the effectiveness of remote triage and 32 studies addressing emerging practices for implementing remote triage systems. No studies specifically addressed Veterans or were conducted in the VA healthcare system. Also, no studies reported modalities of remote triage other than telephone. Summary of Findings 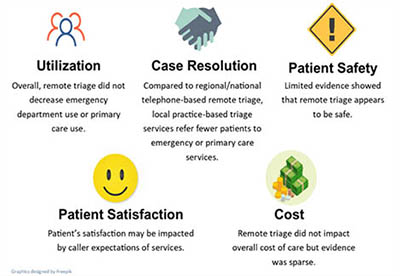
Effectiveness of Remote Triage While the current evidence on the effectiveness of remote triage is limited and of low to moderate certainty of evidence (e.g., few studies, risk of bias issues), the findings of this systematic review hold insights for those wanting to implement such a system.
Emerging Practices for Implementing Remote Triage No studies identified best practices, but focused instead on considerations for emerging practices when implementing a remote triage system in a large-scale healthcare system such as VA.
Implications for Current Practice and Policy Remote clinical triage centers are an increasingly prevalent feature of healthcare delivery, particularly among large healthcare organizations. An important goal for remote clinical triage centers is the ability to provide case resolution during the first contact. Such resolution means that a telephone call is managed without triage for other services – or that a caller is connected with the appropriate individual with only a one-call transfer. An important policy consideration is should the goal of a remote triage system be to resolve cases without triage to in-person services as opposed to determining the appropriate triage destination for that patient? Further, designing a remote triage system has implications related to staffing (clinical vs nonclinical staff), setting caller expectations, and other considerations. For example, having a clinician (e.g., RN) as the first point of contact could allow for dispensing of medical advice, reducing the need for further triage. An alternative staffing model might involve training non-clinicians to make triage decisions (at sites of care that do engage clinical staff). These different design options come with implications for first-contact outcomes and staffing costs. Findings from this review provide insights into considerations for implementing staffing structures to optimize outcomes. Multi-modal contact is another important consideration for VA when designing a remote triage system. The ability to enter the triage system by means other than a telephone call will be important to study and understand. Smartphone-based mechanisms such as texting, messaging, and chat as alternatives to telephone calls may be a preferred means of contact for many Veterans. While the mode that Veterans use to contact the system may be transparent to the recipient, it is nonetheless important to also consider how the recipient receives these requests and what the expectations are for processing requests. Research Gaps/Future Research There is increasing interest among patients and even healthcare systems to provide multiple modes of contact; however, the current comparative literature addressed only telephone contact and in-person modalities. Future interventions should focus on modes of remote triage delivery in addition to telephone (i.e., video, web, mobile applications), the impact of medical record access, the critical elements in support of triage systems, staffing models and experience, and elements of the CDSS (Clinical Decision Support System) that support triage operations. Potential future comparators should include head-to-head comparisons of triage modalities, staffing models, organizational levels, and remote triage features. More research also is needed on the outcomes evaluated in this review. Suggested settings for future research include VA or similar large healthcare systems. Rushton S, Boggan JC, Lewinski AA, Gordon AM, Shoup JP, Van Voorhees E, Whited JD, Alishahi Tabriz A, Adam S, Fulton J, Kosinski AS, Van Noord MG, Williams JW Jr, Goldstein KM, Gierisch JM. Effectiveness of Remote Triage: A Systematic Review. Washington, DC: Evidence Synthesis Program, Health Services Research and Development Service, Office of Research and Development, Department of Veterans Affairs. VA ESP Project #09-010; 2019. View the full report — **VA Intranet only**: |
Related HSR&D Research Topics:
Please feel free to forward this information to others! ESP is currently soliciting review topics from the broader VA community. Nominations will be accepted electronically using the online Topic Submission Form. If your topic is selected for a synthesis, you will be contacted by an ESP Center to refine the questions and determine a timeline for the report. This Management e-Brief is provided to inform you about recent HSR&D findings that may be of interest. The views expressed in this article are those of the authors and do not necessarily reflect the position or policy of the Department of Veterans Affairs. If you have any questions or comments about this Brief, please email CIDER. The Center for Information Dissemination and Education Resources (CIDER) is a VA HSR&D Resource Center charged with disseminating important HSR&D findings and information to policy makers, managers, clinicians, and researchers working to improve the health and care of Veterans. |
|
|
- This report is a product of VA/HSR&D's Evidence Synthesis Program (ESP), which was established to provide timely and accurate synthesis of targeted healthcare topics of particular importance to VA managers and policymakers –; and to disseminate these reports throughout VA. See all reports online. |
||