» Back to list of all Management Briefs

| Issue 167 | February 2020 | ||
|
The report is a product of the VA/HSR Evidence Synthesis Program. Aromatherapy and Essential Oils: A Map of the EvidenceVA is increasing the use of effective new practices and approaches in healthcare as part of its transformation to a more patient-centered healthcare model that focuses on the Veterans’ goals and priorities for their health. The use of various low-risk complementary health interventions also has been increasing both within and outside of the VA healthcare system. Essential oils (EOs) are part of a tradition of herbal medicine dating back thousands of years. EOs are volatile oils that contain the “essence” of an aromatic plant’s fragrance. The therapeutic inhalation of EOs is considered to have physiological and/or psychological benefits. Aromatherapy using EO is thought to mediate emotional responses by affecting the neuroendocrine system and autonomic nervous systems. In addition, there are various topical EO applications that are purported to be beneficial apart from their aromatic qualities (e.g., as antiseptics). The chemical components of EOs also have been shown to inhibit microbial and fungal growth. EO aromatherapy is being used increasingly in hospitals and other healthcare settings. For instance, aromatherapy has been used to help manage the behavioral and psychological symptoms of dementia, such as restlessness and aggression, and to improve sleep. However, despite their increasing use, little is known about the benefits and risks associated with the use of EOs. VA’s Evidence Synthesis Program (ESP) Center in Portland, OR conducted a review to provide VA with a broad overview of the effectiveness of aromatherapy and essential oils (EOs), and the health conditions for which these interventions have been examined. Investigators searched multiple databases from inception through February 2019 for systematic reviews (SRs) of aromatherapy and EOs for health conditions, identifying 25 SRs that were selected for the evidence map (see below): 22 SRs provide evidence on inhaled EO interventions, which encompass aromatherapy combined with massage (EO-massage) as well as inhaled-only aromatherapy, while 3 SRs provide evidence on topical EO interventions. Evidence from 171 eligible trials is represented among the 25 SRs.
This report and evidence map characterize the current knowledge about the effectiveness of inhaled and topical essential oils – and will inform decision-making about these modalities within the VA healthcare system. 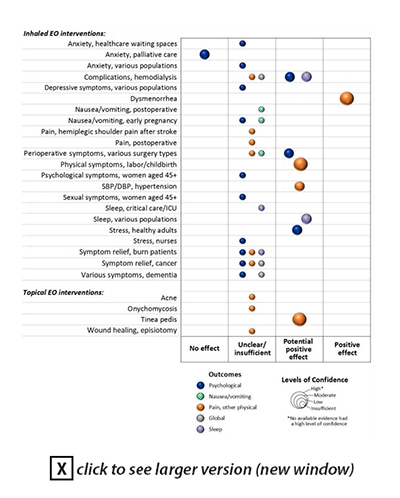 Summary of Conclusions There is moderate confidence that aromatherapy is effective for pain in dysmenorrhea (menstrual cramps). Investigators found potential positive effects of aromatherapy for:
For EOs applied topically, there is moderate confidence in the potentially positive effect of tea tree oil for tinea pedis. There is insufficient evidence with which to determine whether aromatherapy or topically applied EO is effective for all other examined conditions. . Research Gaps/Future Research The evidence map highlights many potential areas for future research. The interventions and health conditions for which there was evidence of a "potential positive effect" may be one place to start to prioritize research. The comparative effectiveness of different, standardized aromatherapeutic approaches should be examined, especially in conditions for which there is potential promise. Future studies should capture potential adverse effects data, and the safety of aromatherapy should be examined in patients with comorbidities, particularly those of the respiratory tract. Also, the use of a non-EO fragrance comparator would improve blinding and allow comparison of effects and harms of aromatherapy containing EO versus synthetically generated fragrance oils. A Cyberseminar titled “Aromatherapy and Essential Oils: An Evidence Map” will be held on March 11, 2020 from 1:00pm – 2:00pm ET. Register here. Freeman M, Ayers CK, Peterson C, and Kansagara D. Aromatherapy and Essential Oils: A Map of the Evidence. Washington, DC: Evidence Synthesis Program, Health Services Research and Development Service, Office of Research and Development, Department of Veterans Affairs. VA ESP Project #05-225; 2019. To view the full report, go to http://www.hsrd.research.va.gov/publications/esp/aromatherapy.cfm |
ESP is currently soliciting review topics from the broader VA community. Nominations will be accepted electronically using the online Topic Submission Form. If your topic is selected for a synthesis, you will be contacted by an ESP Center to refine the questions and determine a timeline for the report. This Management e-Brief is provided to inform you about recent HSR&D findings that may be of interest. The views expressed in this article are those of the authors and do not necessarily reflect the position or policy of the Department of Veterans Affairs. If you have any questions or comments about this Brief, please email CIDER. The Center for Information Dissemination and Education Resources (CIDER) is a VA HSR&D Resource Center charged with disseminating important HSR&D findings and information to policy makers, managers, clinicians, and researchers working to improve the health and care of Veterans. |
||
|
- This report is a product of VA/HSR&D's Evidence Synthesis Program (ESP), which was established to provide timely and accurate synthesis of targeted healthcare topics of particular importance to VA managers and policymakers –; and to disseminate these reports throughout VA. See all reports online. |
|||