» Back to list of all Management Briefs

| Issue 93 | March 2015 |
Mental Health Assessment and Psychosocial Interventions for Bariatric SurgeryObesity rates in the U.S. have risen to near epidemic levels. While the combination of caloric restriction, exercise, and behavioral modification remain mainstays for treating overweight and obese individuals, these strategies have not produced substantial weight loss for the majority of those participating in these comprehensive interventions. Bariatric surgery has become increasingly popular as an adjunctive treatment for Class II or severe obesity, as it has been shown to result in higher rates of sustainable weight loss than non-surgical interventions. However, not all patients receive equal benefit from bariatric surgery. Psychosocial factors are commonly cited as important predictors of post-operative outcomes. Many bariatric practices formally screen for mental health conditions during the pre-operative assessment in order to select patients they believe have the highest likelihood of success; others, including the Veterans Health Administration (VHA), do not require formal psychosocial evaluation. Given the desire to select patients who will benefit the most from this intervention, the Office of Patient Care Services and the Office of Clinical Operations requested a review of the evidence for or against this practice, to help determine if VHA should implement mental health evaluations for bariatric surgery candidates prior to surgery. The review, conducted by the VA Evidence-based Synthesis Program at the West Los Angeles VA Medical Center, concluded that mental health conditions and eating disorders are common in bariatric surgery candidates and patients, in particular depression, anxiety, and binge eating disorders. There is inconsistent evidence about the effect of mental health conditions and eating disorders on subsequent post-operative outcomes, with the exception of improvement in depression and possibly quality of life. There are no studies assessing the effect of pre-operative interventions aimed at mental health conditions or eating disorders. There is insufficient evidence to recommend for or against routine specialized pre-operative mental health screening in bariatric surgery candidates in addition to the prerequisite general evaluation by the surgical and/or medical bariatric team. A partial summary of the findings and evidence quality is outlined in Table 1, below. The review also found differences in the gender of patients assessed in VA compared with non-VA populations – 70% to 80% of non-VA patients are female while 70% to 80% of VA patients are male. The limited VA studies show a higher prevalence of mental health conditions and eating disorders in VA patient populations compared to non-VA populations, thus generalization from the non-VA population to the VA population should be done with caution. In order to generate VA-relevant data, a more broadly-based data collection effort is needed among Veterans seeking bariatric surgery. This should include a sufficient number of sites to be representative of the VA patient population, and use the same standardized instruments for classifying disorders. More research is needed to determine the optimal screening process and helpful interventions to address mental health and eating disorders in bariatric surgery candidates. A protocol for follow-up of such patients could help answer questions about the association between pre-operative mental health conditions and post-operative outcomes. To assess the effectiveness of pre-operative interventions, randomized clinical trials or case-matched cohort studies are needed. 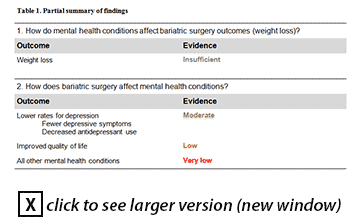
Reference: View the full report — **VA Intranet only**: vaww.hsrd.research.va.gov/publications/esp/bariatric.cfm (copy and paste if you have VA intranet access) |
Please feel free to forward this information to others! This Management eBrief is a product of the HSR&D Evidence Synthesis Program (ESP). ESP is currently soliciting review topics from the broader VA community. Nominations will be accepted electronically using the online Topic Submission Form. If your topic is selected for a synthesis, you will be contacted by an ESP Center to refine the questions and determine a timeline for the report. This Management e-Brief is provided to inform you about recent HSR&D findings that may be of interest. The views expressed in this article are those of the authors and do not necessarily reflect the position or policy of the Department of Veterans Affairs. If you have any questions or comments about this Brief, please email CIDER. The Center for Information Dissemination and Education Resources (CIDER) is a VA HSR&D Resource Center charged with disseminating important HSR&D findings and information to policy makers, managers, clinicians, and researchers working to improve the health and care of Veterans. |
|
- This report is a product of VA/HSR&D's Quality Enhancement Research Initiative's (QUERI) Evidence-Based Synthesis Program (ESP), which was established to provide timely and accurate synthesis of targeted healthcare topics of particular importance to VA managers and policymakers – and to disseminate these reports throughout VA. See all reports online. |
|