 |
MOVE!+UP Behavioral Weight Management Program for Veterans with PTSDHSR&D’s monthly publication Veterans’ Perspectives highlights research conducted by HSR&D and/or QUERI investigators, showcasing the importance of research for Veterans – and the importance of Veterans for research. In the September 2020 Issue:
|
Introduction
MOVE!+UP ProgramSupported by VA's National Center for Health Promotion and Disease Prevention (NCP) the MOVE! weight management program includes the most up-to-date approaches for weight management. MOVE!+UP is tailored to meet the needs of obese and overweight Veterans with PTSD.Posttraumatic Stress Disorder (PTSD), a common mental health condition in Veterans, is associated with increased risk for overweight or obesity, resulting in premature mortality. Despite comparable levels of participation in VA’s national weight management program MOVE!, Veterans with PTSD lose less weight than those not living with PTSD. This may in part be because Veterans with PTSD are at increased risk for inactivity, unhealthy diet, and binge eating. Veterans with PTSD enrolled in the MOVE! program request strategies for managing mental health symptoms and report more barriers to weight loss. Behavioral weight management, which promotes physical activity and healthy diet, may improve both weight and PTSD symptoms among Veterans with PTSD who are diagnosed as overweight or obese. To be most effective, some tailoring of behavioral weight management programs is needed, to address the unique barriers to weight loss experienced by Veterans with PTSD. To meet this need, a team of HSR&D researchers developed and piloted MOVE!+UP, a behavioral weight management program for Veterans with PTSD. Led by HSR&D Career Development Awardee Katherine Hoerster of the Seattle-Denver COIN, MOVE!+UP used the power of Veteran Engagement to build a tailored program. “It’s more thorough...it’s geared specifically for people with PTSD” – MOVE!+UP participant Program Development and TestingBetween 2015-2018, five cohorts of Veterans participated in a single-arm pilot. Based on Veteran feedback, the research team iteratively modified MOVE!+UP between cohorts. Each iteration optimized acceptability and effects on weight, PTSD, and treatment targets such as physical activity, healthy eating, and social support. Cohort 5 Veterans received the fully developed MOVE!+UP intervention. The 16 two-hour MOVE!+UP group sessions provide general weight loss support based on MOVE!, plus Cognitive Behavior Therapy (CBT) skills training, to address PTSD-related barriers. To treat PTSD hypervigilance symptoms that interfere with physical activity, a 30-minute group walk builds experiential comfort with being physically active in the community. Sessions are co-led by a psychologist and a Veteran peer support counselor, and participants receive two individual dietician visits. 
Left: Veteran Peer Support Counselor and MOVE!+UP Facilitator Lamont Tanksley Sr. demonstrates the Community Walks with a Veteran Actor. (Photo Credit: Chris Pacheco) Veteran EngagementVeterans co-created MOVE!+UP by providing ongoing feedback, either as study participants or as a program facilitator. One of the key ways Veterans initiated necessary changes that were integrated into the following iteration of the program was through semi-structured qualitative interviews conducted after the group sessions. Interview topics included impressions of MOVE!+UP content and study procedures, suggestions for improvement, and comparison with MOVE! (among those with MOVE! experience). Additionally, Lamont Tanksley Sr. brought his experience as a Veteran and a Peer Support Counselor to the MOVE!+UP program. Mr. Tanksley not only led MOVE!+UP for all five cohorts, but he provided ongoing input about ways the program should be improved to promote Veteran health and well-being. “It was my goal to lend my skills and experiences as a Veteran…so it can be effectively and successfully delivered by other Veteran peer support counselors in the future” – Veteran Peer Support Counselor Lamont Tanksley Sr. Mr. Tanksley explains: “It was my goal to lend my skills and experiences as a Veteran, whole health coach, and peer support counselor to the MOVE!+UP content, analysis, and facilitation methods,” His active participation shaped how the program promotes Veteran health and well-being and how future peer support counselors will deliver MOVE!+UP. Lamont was guided by the perspective that “it’s not enough for the program to be able to generate successful health outcomes for study participants. It also has to be structured so it can be effectively and successfully delivered by other Veteran peer support counselors in the future.” To that end, the program has taken input—every step of the way—from Veteran participants and Mr. Tanksley to improve the content and approach. He co-authored the journal article describing pilot results in the American Journal of Health Promotion, and will be heavily involved in the upcoming HSR&D-funded randomized controlled trial. 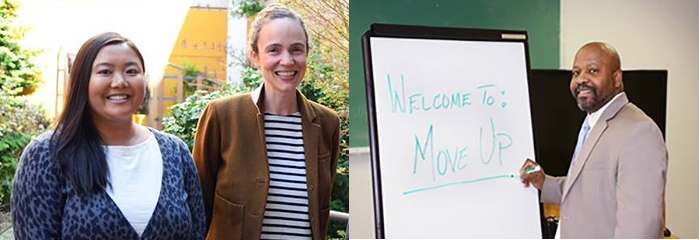
Left: Research Coordinator Nadiyah Sulayman and Principal Investigator Kate Hoerster, PhD, MPH. ImpactThe final cohort reported high satisfaction with MOVE!+UP. They also showed meaningful weight and PTSD improvements. More than 70% of Veteran participants lost approximately 5% of baseline weight, with an average decrease of 14 lbs. PTSD symptom severity as measured on the PTSD Checklist was down by nearly 18%. Significant improvements were also observed for insomnia and eating behaviors. MOVE!+UP delivered as an adjunct to standard PTSD care holds promise for better promoting weight loss and PTSD symptom reduction than standard VA MOVE! and PTSD care alone. Here is what several Veteran MOVE!+UP participants had to say about their experience with MOVE!+UP: “I think it really did help. It showed me that I could do it.” “My..eating..changed, my physical activity..changed…now it has become a habit” “It opened up my eyes to how I was eating ... Basically, if I was getting..depressed or into my thoughts, or being alone or with the PTSD..I’d eat more.” “Besides just the support, knowledge and positive feedback that they gave us, they were just people that I trusted, which says a lot for someone with PTSD.” “[It helped me]… get me out of my shell…and interact with other people that are suffering from PTSD too.”
Katherine D. Hoerster, PhD is an Investigator at the Seattle-Denver Center of Innovation (COIN) for Veteran-Centered and Value-Driven Care.Next StepsFunding for continued research has been approved. A randomized controlled trial of MOVE!+UP is slated to begin later in 2020. The study will test whether intervention participants have greater 6-month weight loss (primary outcome), and 6-month PTSD symptom reduction and 12-month weight loss (secondary exploratory outcomes), relative to those randomized to receive the MOVE! program only. If MOVE!+UP is effective, it would be positioned to address top VA priorities of improving obesity and PTSD among Veterans. This study also will have broad implications for VA weight management and PTSD care. |