 |
Engaging Family Supporters to Improve Veterans’ Diabetes Care: The CO-IMPACT Program and ToolkitHSR&D’s monthly publication Veterans’ Perspectives highlights research conducted by HSR&D and/or QUERI investigators, showcasing the importance of research for Veterans – and the importance of Veterans for research. In the October 2021 Issue:
|
Introduction
CO-IMPACT study principal investigator Ann-Marie Rosland MD, MS, is with HSR&D’s Center for Health Equity Research and Promotion (CHERP) in Pittsburgh, Co-Principal Investigator of the RIVET Quality Enhancement Research Initiative (QUERI) Program and Director of the VA Primary Care High Risk Patient Care Network.
Type 2 diabetes is a common condition among Veterans. Veterans with diabetes are at risk for disabling complications including stroke, heart attack, amputation, kidney failure, and blindness. Following treatment plans and actively managing diabetes day-to-day will reduce the risk of complications, but it can be challenging to stick to complicated regimens. Veterans with diabetes also often need to coordinate care with multiple specialists and arrange regular testing to stay their healthiest. Research has shown that Veterans who have diabetes care support from family and friends are more confident and successful in managing diabetes. Current guidelines for diabetes education call for healthcare teams to engage these ‘family supporters’ in diabetes care. However, clear and effective ways to involve them have not been developed. To help Veterans and their care teams tap into this source of support, a team of HSR&D researchers at the Pittsburgh and Ann Arbor VA Healthcare Systems, led by Ann-Marie Rosland MD, MS, developed the Caring Others Increasing Engagement in Patient Aligned Care Teams (CO-IMPACT) program. 
CO-IMPACT team members (left to right) Lindsey Street, Ann-Marie Rosland, Shelley Stoll, and Keosha Corder in 2016. Developmental ResearchTo develop the CO-IMPACT program, Dr. Rosland and colleagues started by surveying and interviewing Veterans with complex diabetes and their family supporters. In a survey of over 550 Veterans with complex diabetes, 47% said they brought a family supporter to their medical appointments on a regular basis. Many of those Veterans wanted their supporter to be able to provide information to their doctor even if they couldn’t come to an appointment, and to have access to the results of their medical visits and tests. Among the Veterans with a supporter involved in diabetes care at home, 90% brought their supporter with them when they attended diabetes-related group programs or classes. Most also said their supporter helped them manage VA appointments and navigate VA services. In interviews, Veterans with complex diabetes and their family supporters described preparation and review activities before and after medical visits: Veteran: “We usually go through my meds and stuff before a visit then during a visit I will go through my medications one by one with the doctor…Sometimes I’ll tell [supporter] things and then I’ll forget and she’ll say ‘Don’t forget to ask them about…’” Supporter: “I ask him, ‘Dad, did you understand what they were talking about? If you don’t, well, here’s what I took this to mean,’ and we’ll break it down and we’ll work on it.” When asked what would help them be more effective, supporters reported feeling limited by a lack of patient-specific information, such as changes in medication regimens or test results, as well as a lack of health system-specific information, such as VA healthcare provider roles, or available diabetes programs. They also wanted to learn positive ways to encourage and help Veterans adopt more healthy lifestyles. Importantly, very few Veterans (9%) in the study survey felt that privacy should be a barrier to information sharing between their supporters and clinicians. Pilot Program
"The program was an eye opener for me about what was needed to manage diabetes vs. what we were actually doing" - CO-IMPACT pilot program participant.
Based on recommendations from Veterans and their supporters, the study team developed a pilot program. Twenty Veterans and their supporters - now called “Care Partners”- participated. Results were very encouraging:
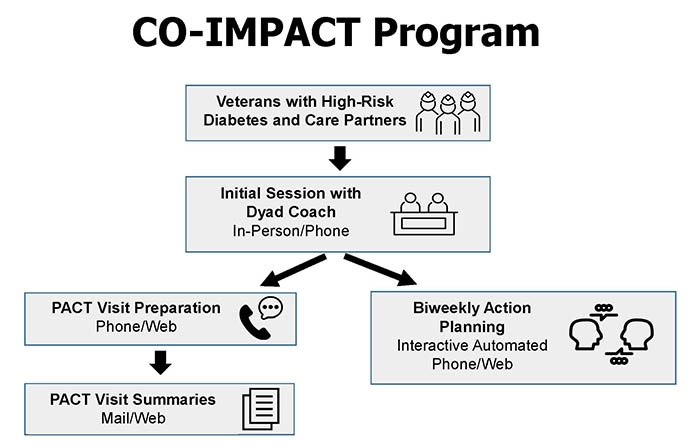
CO-IMPACT ProgramAfter incorporating feedback from pilot study participants, the team conducted a larger trial with 240 Veteran-Care Partner pairs randomized to the CO-IMPACT program or usual primary care for one year. The full program, successfully implemented at two sites, included:
All parts of CO-IMPACT emphasized how Care Partners could support Veteran autonomy and ownership of diabetes management. The program also emphasized how Care Partners could support Veterans in being active and engaged participants in their healthcare. ImpactsRecruitment, Engagement, and Retention: The CO-IMPACT study was extremely successful in recruiting and engaging Veteran-caregiver pairs. Study investigators have gained novel insights into increasing caregiver engagement in VA care that will be helpful to other researchers. Impact on Veteran and Care Partner Diabetes Management: Veterans in CO-IMPACT had a significantly larger increase in the study’s primary outcome – patient activation – than those in usual primary care. ‘Patient activation’ includes the ability to self-manage and engage in activities that maintain health, to actively get involved in treatment choices, and to have the ability to collaborate with healthcare providers and navigate the health care system. Veterans in the CO-IMPACT program also significantly improved their diabetes self-efficacy and healthy eating. Structured chart review revealed that the automated voice response calling system identified urgent diabetes issues that were addressed by PACT teams virtually between patient visits. Care Partner involvement in key diabetes home care tasks, such as helping to remember to take and fill medications, significantly increased in the intervention arm compared to control. Care Partners in Co-IMPACT also increased their help navigating the health care system, including help using the “MyHealtheVet” patient health portal. Finally, Veterans in CO-IMPACT reported their Care Partners used positive communication techniques when discussing diabetes more often than those in the comparison group. Veteran Satisfaction: Investigators received very positive feedback from users on materials and the program. 94% of Veterans and 83% of caregivers reported the program helped the Veteran improve their diabetes management. Veterans reporting that they were satisfied with VA support for involving their caregiver in their healthcare rose from 53% to 84% in the intervention group. 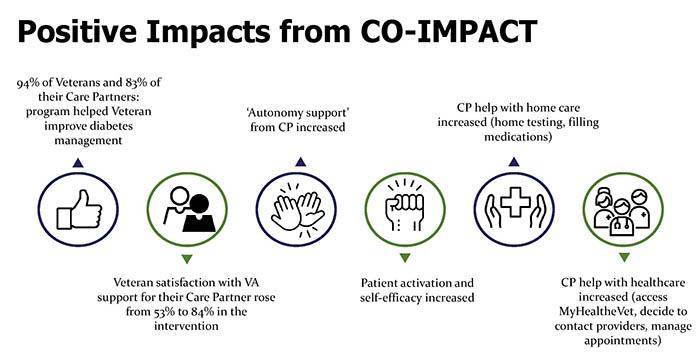
Several participants shared what they learned through the CO-IMPACT program: “Beforehand, she and I did not talk as much about my diabetes … but as we had specific coaching it helped us talk about it every night, even if she was traveling.” “It put [us on the] same plane on managing diabetes, making sure we have a well-rounded diet and taking my metformin at a specific time every day.” “It helped us look at it from a different perspective and put more emphasis on… doing what we needed to do …and realize the only people that could really do it was us.”
The Center for Health Equity Research and Promotion (CHERP) focuses on detecting, understanding, and reducing disparities in health and health care in vulnerable populations. CHERP investigators and staff partner with VA operations and policy leaders to implement research results and disseminate research findings to improve the clinical care and health outcomes of Veterans.
Next StepsDue to its success in increasing Veteran and Care Partner engagement in diabetes care, the team was granted additional HSR&D funding to disseminate tools and strategies developed in the CO-IMPACT program to Veterans, Care Partners, and VA healthcare providers. The team used feedback from program participants and staff to develop web-based toolkits for two audiences. The toolkit for Healthcare Professionals includes descriptions of all CO-IMPACT sessions and tools, how the tools were used in the original program, and tips on how they can be used in other settings. The other toolkit, developed for Veterans and Care Partners, includes information on how supporters can help with specific diabetes self-management tasks, how to work as a team with Veterans, including using positive communication techniques, and printable worksheets and logs. The team is now partnering with VA Primary Care and Caregiver Support Programs to get the tools into the hands of providers, Veterans, and family supporters who can use them. CO-IMPACT Toolkits can be found at: https://www.complexcaring.pitt.edu/co-impact-toolkit |