
|
|
Research HighlightFeedback Reports Expected to Improve Implementation of the Life-Sustaining Treatment Decisions Initiative in VA Long-term Care SettingsKey Points
In January 2017, the National Center for Ethics in Health Care (NCEHC) updated guidance for initiating and documenting conversations and decisions made by seriously ill Veterans regarding preferences for care, specifically life-sustaining treatments.1 NCEHC designed the Life-Sustaining Treatment Decisions Initiative (LSTDI) to ensure that Veterans’ goals, values, and preferences for life-sustaining treatments are elicited and documented in the electronic medical record using the life-sustaining treatment template. Goals of care conversations (GoCC) help guide proactive conversations about options and Veterans’ preferences for life-sustaining treatments such as artificial nutrition, ventilator support, and cardiopulmonary resuscitation; clinicians conduct GoCCs prior to a life-limiting or life-threatening event. The Implementing Goals of Care Conversations with Veterans in VA Long-Term Care Settings Quality Enhancement Research Initiative (LTC QUERI program) supports the implementation of the LSTDI in Community Living Centers (CLCs) and Home-Based Primary Care (HBPC) in three VHA VISNs.2 The LTC QUERI program chose these care settings because Veterans using these services are often seriously ill and thus appropriate for a GoCC and documented LST preferences. As part of our work, we send regular feedback reports to CLC and HBPC sites in VISNs 4, 10, and 19. These reports show the number of newly admitted Veterans who have a documented GoCC and who have completed Life-Sustaining Treatment (LST) documentation with their provider. These Veteran-level data are extracted from the VHA’s Corporate Data Warehouse (CDW). Prior to finalizing the feedback reports, we conducted an iterative user-centered design process to create and refine the content and format of the reports. Monthly production of our feedback reports is now automated using SQL code to extract data from CDW; SAS code for data management and analysis; and code written in R programming language to produce reports in pdf format. Our iterative design process led to several changes following distribution of the reports in July 2017. These changes included increasing the frequency of reports from quarterly to monthly, showing separate data for short-stay vs. long-stay Veterans in CLCs, and updating language to be consistent with what is being used in the field regarding LSTs. The feedback reports are sent to a designated site champion or champions who are asked to distribute the reports more widely, based on their preferences and local knowledge. Site champions are leaders within these care settings, whether formal or informal, who agree to serve as liaisons for our work. The monthly feedback reports are currently sent to 28 CLCs and HBPC programs. Site champions at 16 of the programs/CLCs share the reports; that is, the champions provide an electronic or hard copy to CLC or HBPC staff, leadership, LSTDI advisory boards and coordinators, and/or others in their facility. The other sites are either in the beginning stages of sharing reports or have stated that they are not sharing widely due to late adoption of the LSTDI, lack of prescribing providers available to complete GoCC, or have other site-specific reasons for not sharing. Between July 2018 and April 2019, 3,434 documented GoCC and LST orders have been recorded at the CLC and HBPC programs in which we are engaged. Of these conversations, 2,283 (67 percent) occurred in the CLC and 1,151 (33 percent) occurred in HBPC. We expect that our feedback reports will result in more completed LSTDI templates at our participating sites compared with a matched sample of non-participating CLC and HBPC programs. Our analysis will focus on Veterans who are newly admitted to a CLC or HBPC. We plan to begin this analysis in April 2020, which will allow us to examine outcomes of the feedback reports over a two-year period. Lessons learned from the LTC QUERI program are regularly communicated to the NCEHC through monthly teleconferences. These lessons have helped to inform the national roll out of the LSTDI. We are currently partnering with the NCEHC to develop approaches to enhance successful implementation of GoCC and their documentation across the system. 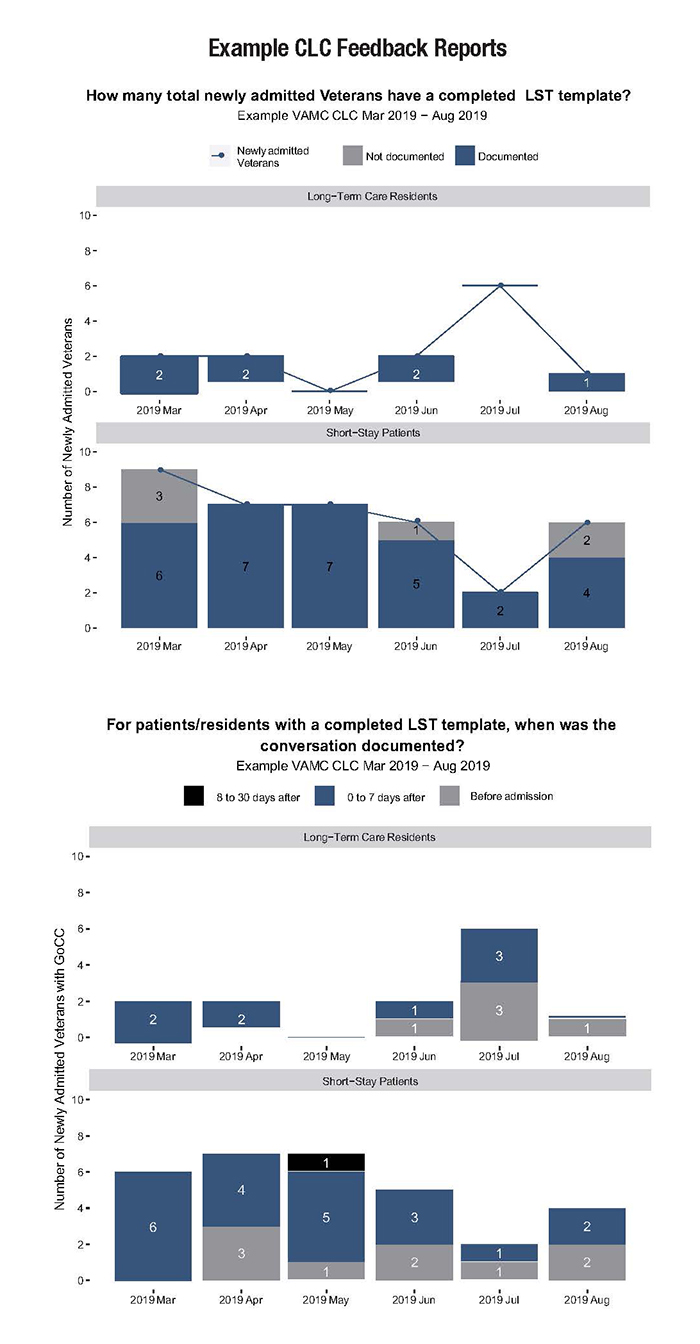
References
|
|