 |
Majority of Women Veterans Feel Welcome at VAHSR&D’s monthly publication Veterans’ Perspectives highlights research conducted by HSR&D and/or QUERI investigators, showcasing the importance of research for Veterans – and the importance of Veterans for research. In the July 2020 Issue:
|
IntroductionWomen's Health Practice-Based Research NetworkThe WH-PBRN is part of the VA Women’s Health Research Network (WHRN), which was initially funded by HSR&D in 2010 to promote evidence-based innovations for the healthcare of women Veterans by developing a PBRN and a national Consortium of VA researchers to conduct women Veteran’s health research. The focus of the WH-PBRN was – and is – to facilitate the recruitment of women Veterans in VA research. As of 2019, more than 47 projects and studies have used WH-PBRN resources.Women Veterans are a rapidly increasing subset of VA’s patient population. From 2005 to 2015, the number of women Veterans using VA healthcare increased by 46%; however, women Veterans remain a minority patient population at about 7.5% of patients. The dominant presence of male patients in VA healthcare settings poses unique considerations for providing care in a setting or manner that makes women feel welcome. In response, VA escalated ongoing efforts to ensure that women Veterans experience an environment in which they feel safe, welcome, and respected, and actively sought women Veterans’ input on these efforts and potential future changes. As part of these efforts, investigators conducted a study that analyzed patient suggestions on how to make the VA healthcare system more welcoming to women. In August and September 2017, a survey was given to a convenience sample of women Veterans (n=1,303) at 26 VA primary care and women’s clinics that were part of VA’s Women’s Health Practice-Based Research Network (WH-PBRN). Women Veterans who attended participating clinics were invited to complete the voluntary survey, which included yes/no questions about whether they felt welcome within VA, and whether they had experienced harassment at VA (e.g., sexual remarks, unwanted attention). In addition, investigators gathered basic patient demographics (i.e., age, number of VA visits in the past year), which, overall, correlated with women Veteran VA users. Study findingsLed by Ruth Klap, PhD, part of HSR&D’s Center for the Study of Healthcare Innovation, Implementation and Policy (CSHIIP) in Los Angeles, CA, in partnership with WH-PBRN investigators, this study found that 85% of the women Veteran study participants felt welcome within the VA healthcare system, with 15% feeling neutral or unwelcome. The survey concluded with an open-ended question that solicited participants’ suggestions for making VA more welcoming to women Veterans, and 490 responses were offered (260 comments and 230 suggestions). Comments included praise for VA (67%), as well as stories about feeling uncomfortable or harassed within VA (26%). Following are some of the women Veterans’ individual responses. 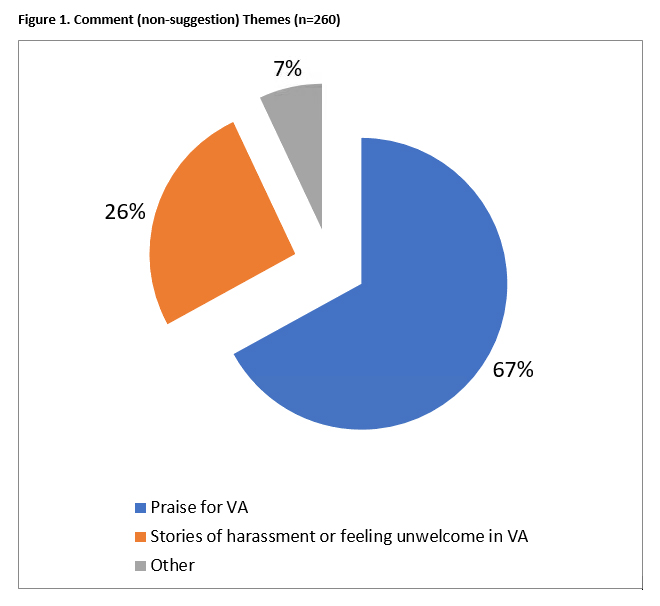
Praise for VA“I am very grateful for all the outstanding care I have received. You, the women’s clinic, are doing a great job!” “I have been coming here since my separation date [from the military] and since then a great deal has changed in help for female veterans and I am very pleased.” “I always have a great experience at the women’s clinic.” Stories about feeling uncomfortable or harassed at VA (26% of comments)“Sometimes male veterans stare at me and I wonder why. Are they thinking I don’t belong here? Maybe they mean nothing. It’s uncomfortable if it goes on. Once another male vet pressured me really hard for a date even though I told him I already had a boyfriend. I felt a little scared and very uncomfortable.” “I mainly noticed at this VA groups [of male Veterans] hanging out at the entrances smoking. It was scary and they would constantly make comments as I walked by. It makes me extremely uncomfortable that men hang out at the entrances.” “Too many vets have no respect which makes me mad and feel like I don’t want to be here or walk around.” Suggestions by Women VeteransSuggestions for making VA more welcoming to women (31% of suggestions pertained to VA staff)“Try to retain more female staff and support personnel. This would really help reduce the level of anxiety as a female veteran to be surrounded by [women].” “Through training for staff about appropriate ways to welcome someone in. No more “does your husband have an appointment.” “Don’t call us sir! This does not happen in the women’s clinic – they are awesome – but other areas of the hospital automatically default to sir. Very disrespectful.” Environment of care (18% of suggestions)“The women’s center needs to be separate with its own entrance, child care, and staff.” “Have volunteers in hallway[s] listening for harassment.” Additional resources for women Veterans (15% of suggestions)“Invite women vets who are being seen at VA to events hosted by the VA in an attempt to inform female vets to many of the VA services. Help familiarize female vets with all the VA has to offer.” “Need to see more posters [of women Veterans] not just about women serving. It helps to engrave the message that YES we are here.” Clinical services for women Veterans (15% of suggestions)“The women’s clinic offers great services, but I wish an OB/GYN would be available on a more consistent basis. I scheduled an appointment but was told I would have to wait 1+1/2 months. Very sad.” Making treatment of women and men Veterans the same (5% of suggestions)“I spent my entire career wearing the same uniform [as men] with equal treatment. I don’t want to be called out or have my gender be an issue. I want to be treated the same – equal. No special treatment.” 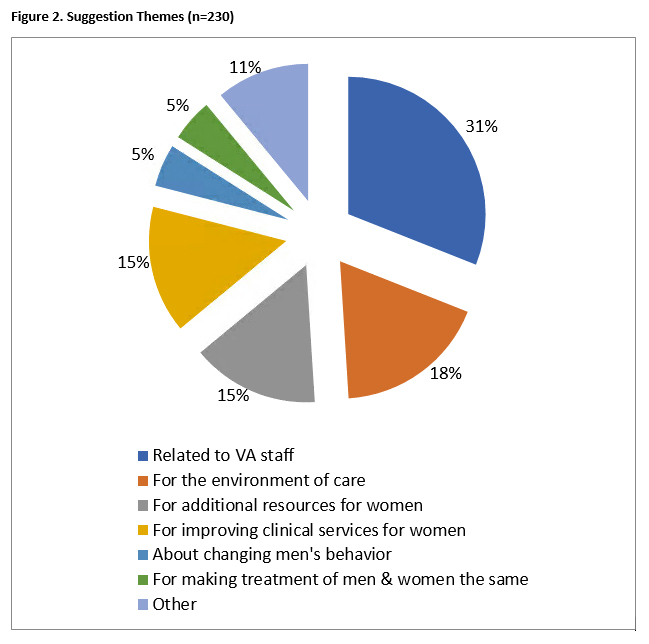
Proportion of themes from the 230 suggestions made by women Veterans on how to make VA more welcoming to female patients. Policy implicationsAs a learning healthcare system, efforts to make VA more welcoming to women support VA’s commitment to be constantly learning and improving. Given that many respondents identified staff gender sensitivity as an area in need of improvement, further attention should be paid to staff training, especially for new staff who may be unfamiliar with the male-dominated VA environment. Policies related to addressing harassment at multiple levels also should continue to be developed and implemented. To read more about this study, see: Moreau J, Dyer K, Hamilton A, Golden R, Combs A, Carney D, Frayne S, Yano E, Ruth Klap, and the VA Women’s Health Practice-Based Research Network. Women Veterans’ Perspectives on How to Make Veterans Affairs Healthcare Settings More Welcoming to Women. Women’s Health Issues. April 24, 2020; Epub ahead of print. This project was conducted by the HSR&D-funded Women’s Health Practice-Based Research Network and was done at the request of VA Women’s Health Services. In addition, HSR&D funds various other studies focusing on women’s health, including but not limited to: Addressing Gender-Based Harassment of Women Veterans at VA Facilities; Reproductive Planning for Women Veterans; Connecting Women to Care: Home-based Psychotherapy for Women with MST Living in Rural Areas; Attrition of Women Veterans New to VHA in the Community Care Era; and Addressing Intimate Partner Violence among Women Veterans. HSR&D also supports the Enhancing Mental and Physical health of Women through Engagement and Retention (EMPOWER) QUERI program. |