Complementary and integrative health (CIH) consists of treatment approaches that are not currently part of conventional medical practice and may be considered complementary, thus used in place of or along with standard medical care. Integrative medicine refers to care that blends both mainstream and alternative practices. CIH emphasizes patient empowerment, self-activation, preventive self-care, and wellness1.
In May 2017 the Under Secretary for Health (USH) approved VA Directive 1137 - Provision of Complementary and Integrative Health, establishing national VA policy regarding the provision of CIH approaches. Since that time VA has developed the policy and guidance required to implement CIH services that meet the definition of basic care as described in the standard Medical Benefits Package and that are in accord with generally accepted standards of medical practice. The CIH approaches that can be included in the Veterans’ medical benefits package if deemed appropriate by their care team include:
These approaches are most often used to treat Veterans’ mental health, manage pain, and promote general wellness. More specifically, these approaches are often used to treat PTSD, depression, back pain, headache, arthritis, fibromyalgia, and substance abuse.
One of the greatest challenges in CIH is critically assessing the effectiveness of treatments that have not been rigorously tested through formal research. HSR&D researchers remain committed to addressing these scientific gaps. They are conducting studies to determine which approaches are truly safe and effective, and for which conditions and populations they work best. Evaluations of access, efficacy, and benefits vs costs3 make up the majority of research into CIH at VA. Below are several examples.
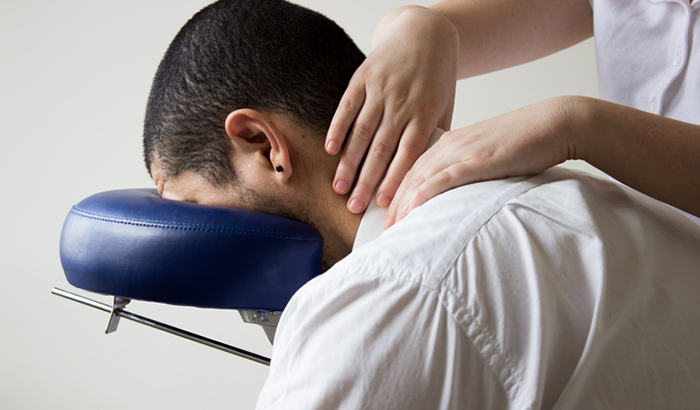
©iStock/Alice Gaudioso
Implications:
This project addresses pain, an important VA priority area, using a novel care delivery approach. It has strong implementation potential and innovates by placing caregivers in a treatment delivery role that has the potential to reach a greater number of Veterans with chronic neck pain while also producing substantial cost savings.
Overview:
Neck pain is common in adults older than 50 and is the fourth leading cause of disability in the United States. In a 2008 VA study, Dobscha et al. found that back and neck pain diagnoses were present in 67% of Veteran participants. In Veterans with cervical stenosis and disk herniation, neck pain was reported by 96%. Chronic neck pain reduces functional status and quality of life and is associated with depression and anxiety. Chronic neck pain also is a major reason for health care utilization, accounting for more than 10 million ambulatory medical visits per year.
In a national survey, 61% of individuals with neck pain who used both complementary and conventional treatments perceived complementary therapies to be more helpful, whereas only 6% perceived conventional treatments to be better. In a review of complementary health approaches for neck pain, massage reduced pain and/or disability more than usual medical care (such as NSAIDs and exercise), physical therapy, or no treatment. Other systematic reviews have shown massage to be effective in the short term for neck pain, but long-term benefits are unclear. Furthermore, massage is frequently perceived by patients as helpful. Massage is theorized to work through a variety of mechanisms to relieve pain, including increased blood flow and joint flexibility, improved muscle tone, and heightened relaxation response.
The national average $60/hour cost for massage therapy is primarily an out-of-pocket expense that is rarely covered by health insurance and not affordable to most Veterans. While massage therapy is offered at some VA care settings it is not widely available to Veterans. Teaching informal care allies to provide massage has been most commonly applied and found effective for patients with cancer. Care-ally delivered massage has also been tested in the context of pediatric, obstetrical, and long-term care settings for dementia. Massage from caregivers has been shown to lead to decreases in patients' pain, depression, and other cancer-related symptoms. In addition, caregivers benefitted from doing active, hands-on massage. Care-ally delivered massage has not been tested in Veterans with chronic non-cancer pain.
This study sought to:
1) Compare the effects of two massage interventions (care-ally-assisted massage (CAM) and therapist-treated massage (TTM) vs. waitlist control (WLC) on pain-related disability.
2) Compare the effects of the two massage interventions vs. control on secondary outcomes, including pain severity, health-related quality of life, depression, anxiety, and stress.
3) Examine the implementation potential of both massage interventions, including facilitators and barriers, treatment and adherence, and intervention costs.
The study design targeted 468 Veterans with chronic neck pain who had a care-ally willing to learn and provide massage therapy, divided into 156 dyads each for 3 arms (two massage interventions and the waitlist control). The intervention period lasted 3 months and outcomes assessments were completed at baseline, 1, 3, and 6 months. The CAM intervention consisted of an in-person training workshop, and both a written treatment manual and DVD recording with images to serve as a references for participants. Participants were asked to engage in at least 3 care-ally-assisted massage sessions every week at home for the 3-month intervention period and to record their massage activity in a provided study log.
Study Updates:
Preliminary Findings:
Principal Investigator: Matthew J. Bair MD, MS, is an investigator with the Center for Health Information and Communication (CHIC) in Indianapolis IN.
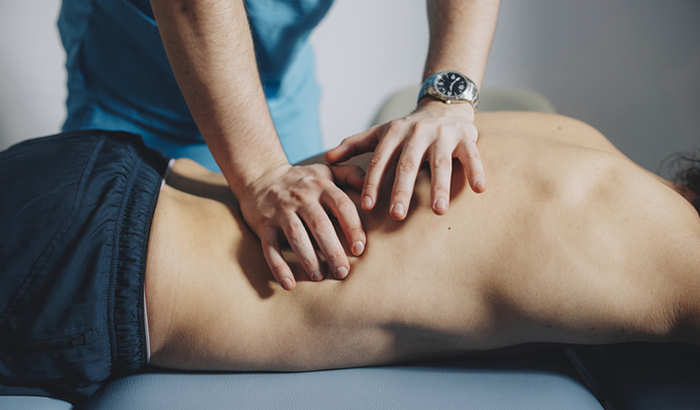
©iStock/miniseries
Implications:
This study is the first large-scale examination of the effects of complementary and integrative health (CIH) therapy use on pain and comorbid outcomes among Veterans and examines the effectiveness of practitioner-delivered CIH therapies in combination with or instead of CIH self-care.
Overview:
More than half of Veterans report musculoskeletal pain, often with mental health comorbidities. Complementary and integrative health (CIH) therapies (i.e., massage, yoga, acupuncture) are important non-pharmacologic treatment options for these conditions. Practitioner-delivered therapies such as acupuncture, chiropractic and therapeutic massage are promising, but providers would like patients to be more active in their pain management by using self-care instead of relying on practitioner-delivered care. A critical question for the field is whether adding self-care CIH to practitioner-delivered CIH is a more effective approach than either strategy alone.
The APPROACH Trial is examining the effectiveness of practitioner-delivered CIH combined with self-care CIH versus practitioner-delivered care alone among Veterans with chronic musculoskeletal pain. It aims to improve Veterans’ pain, several pain-related comorbid conditions, and opioid use. The study is being conducted at the 18 Whole Health Flagship VAMCs in partnership with the VA Office of Patient Centered Care and Cultural Transformation (OPCC&CT).
Investigators are conducting the two-arm pragmatic trial to assess the effectiveness of practitioner-delivered care (acupuncture, chiropractic care, or therapeutic massage) combined with self-care (Tai Chi/Qigong, meditation/mindfulness or yoga) versus practitioner-delivered care alone. The primary outcome measure is the change from the index visit to six months in paint interference and severity. Secondary outcomes include improvement in pain, mental health, physical health, fatigue, and overall well-being. Outcomes will be examined at 3 and 6 months for 5,220 Veterans using CIH. The analysis will use an instrumental variable approach, to take advantage of the variation in the "nudges" that sites use to encourage Veterans to try self-care CIH therapies.
Study Updates:
Publications:
Zeliadt S, Coggeshall S, Thomas E, et al. The APPROACH trial: Assessing pain, patient-reported outcomes, and complementary and integrative health. Clinical Trials. August 17, 2020(4):351-359.
Zeliadt S, Gelman H, Shin M, et al. Assessing the relative effectiveness of self-care and provider-delivered CIH therapies to improve pain in a pragmatic trial. Pain Medicine. December 12 2020; 21(S2): S100–S109.
Principal Investigators: Stephanie L Taylor, PhD, MPH, co-leads QUERI’s Complementary and Integrative Health Evaluation Center (CIHEC) and is Senior Investigator with the Center for the Study of Healthcare Innovation, Implementation and Policy (CSHIIP) COIN in Los Angeles CA. Steven B. Zeliadt, PhD, MPH, is Associate Director of the Veteran-Centered and Value Driven Care Center of Innovation (COIN) in Seattle WA.
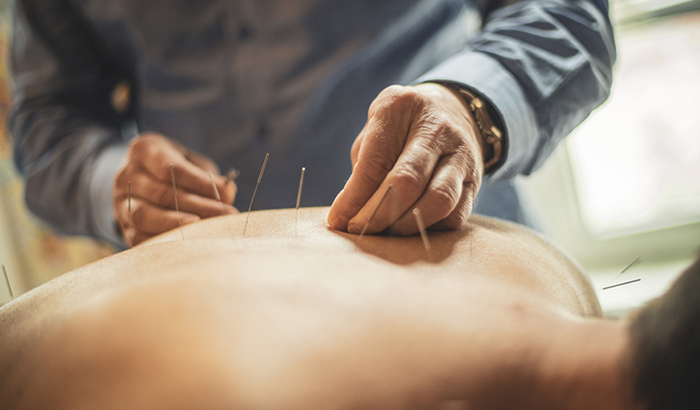
©iStock/LukaTDB
Implications:
Despite the adverse impact of opioid use on Veterans with pain, there is limited evidence of the effect of complementary and integrative health (CIH) use in this population. CIH interventions are used for the treatment of pain. None have been evaluated for their effectiveness in reducing opioid initiation, nor whether the effect varies by Veteran demographic and/or clinical characteristics, or whether they are associated with worse pain-related outcomes, such as new depressive disorder diagnoses.
Overview:
Opioids misuse, abuse, addiction, and overdose have become serious public health issues worldwide. They are also a leading cause of death in the US. Complementary and integrative health (CIH) interventions may help prevent or reduce opioid-related harms. However, an April 2016 Evidence Synthesis Program (ESP) report stated that "the evidence base regarding the effectiveness of select CIH interventions for reducing opioid use is extremely limited." Strategies to identify CIH use and its effects are needed.
Because Veterans with PTSD are at higher risk for opioid related harms, and because of the potential mutual reinforcement of PTSD and pain symptoms, CIH may have substantial impact on decreasing rates of opioid initiation and harms. This study sought to examine CIH use and non-use among Veterans with musculoskeletal disorders (MSD) and compare opioid and pain outcomes by PTSD status.
Study aims were to:
Investigators used algorithms from the Musculoskeletal Disorders cohort study (CRE 12-012) to identify Veterans with MSD, and assess CIH use via structured data such as procedure and ICD codes, and informatics tools on unstructured data (clinical notes). They examined acupuncture, massage, meditation/mindfulness and yoga as they are currently or likely to be integrated into routine VA care. Using structured data only, study investigators identified 7,621 CIH users among MSD cohort entrants in FY11-FY13 (n= 309,277); of which, 21% had a PTSD diagnosis. Opioid and other medications were identified from pharmacy data.
Preliminary Findings:
Principal Investigator: Joseph L. Goulet, PhD, MS, is an investigator with the Pain Research, Informatics, Multi-morbidities, and Education (PRIME) Center in West Haven, CT.

©iStock/jacoblund
Implications:
The interim study findings demonstrated the effectiveness of the Trauma Center Trauma-Sensitive Yoga (TCTSY) intervention in reducing PTSD symptom severity and superior treatment completion rates compared to CPT. This study may yield meaningful data to support clinical guidelines for a complementary and alternative medicine intervention that is more acceptable to women Veterans with PTSD related to military sexual trauma than other treatments. TCTSY is scalable and could be implemented in VA Medical Centers nationwide, thus improving the quality of care for women Veterans with PTSD who experienced sexual trauma.
Overview:
Military sexual trauma (MST) is reported by at least 38% of women military service members and Veterans. MST is the most common cause of PTSD among women Veterans and is strongly associated with co-occurring depression and chronic pain. Although there are evidence-based, cognitively-oriented, trauma-focused psychotherapies for PTSD, not all individuals respond or agree to participate in these, therefore new treatments from innovative theoretical perspectives are needed. Emerging research evidence suggests that yoga is an effective therapeutic intervention for PTSD, particularly in men who experienced combat trauma. However, this body of research examining the beneficial effects of yoga for Veterans with PTSD is limited by methodological problems, under-representation of women, and lack of consideration of sexual trauma. In this study, researchers investigated a novel yoga approach to treat PTSD and associated symptoms, including chronic pain and insomnia, which appear to be the most intractable symptoms associated with MST and PTSD. The theoretical framework suggests that a trauma-sensitive yoga intervention will reduce PTSD symptoms, chronic pain, and insomnia via psychophysiological mechanisms, rather than the cognitive mechanisms of current psychotherapeutic treatments.
The objectives of this study were to:
Participants were randomly assigned to either the Intervention Group, receiving 10 sessions of TCTSY or the Control Group, receiving 12 sessions of CPT. Two hundred women Veterans were recruited from the Atlanta VA Health Care System and the VA Portland Health Care System.
Study Updates:
Publications:
Kelly U, Haywood T, Segell E, Higgins M. Trauma-sensitive yoga for post-traumatic stress disorder in women veterans who experienced military sexual trauma: interim results from a randomized controlled trial. Journal of Alternative and Complementary Medicine. 2021 Mar 27:S45–S59.
Zaccari B, Loftis J, Kelly U, et al. Synchronous Telehealth Yoga and Cognitive Processing Group Therapies for Women Veterans with Posttraumatic Stress Disorder: A Multisite Randomized Controlled Trial Adapted for COVID-19. Telemedicine and E-Health. 2022 Mar 29. Epub ahead of print.
Principal Investigator: Ursula Ann Kelly, PhD, MSN, APRN, FAANP, FAAN is an investigator with the Atlanta VA Health Care System, Decatur, GA.