Part of HSR&D’s Center for Innovations in Quality, Effectiveness and Safety (IQuESt) based at the Michael E. DeBakey VA Medical Center in Houston, TX, Hardeep Singh, MD, MPH, and his Diagnosis Improvement Safety Center (DISCovery) team were awarded the 2016 HSR&D Health System Impact Award for conducting research that has had a significant policy and practice impact on improving patient safety in the VA outpatient setting.
Background
Dr. Singh leads an internationally recognized multidisciplinary team with a shared goal of reducing missed and delayed diagnoses in healthcare. The team includes experts from cognitive psychology, computer science, human factors engineering, social sciences, internal medicine, and clinical informatics and is supported by HSR&D and the VA National Center for Patient Safety. Since 2007, the team has conducted research to improve communication of test results, identify and reduce diagnostic errors, and improve the safety of care using VA’s Computerized Patient Record System (CPRS). Dr. Singh and his team have developed several types of innovations to impact the VA healthcare system, including trigger tools to identify patients with missed or delayed follow-up of test results, safety assessment guides for electronic health records (EHRs), and decision-support software for the EHR, all of which aim to improve diagnostic safety and outcomes of EHR-based communication.
Impact
The team’s impact on policy and practice in the VA healthcare system includes initiatives to measure and improve communication of diagnostic test results to patients and clinicians. The team partnered with VA operations leaders to help develop and disseminate several guidance documents for the field, including three toolkits to help frontline clinicians safely manage ‘alert’ notifications of test results in the EHR. For example, the Communication of Test Results toolkit has been distributed to all 150+ VA facilities and their clinicians – an audience of about 250,000. In addition, Dr. Singh co-developed the national VA policy on communication of test results to patients and providers. This policy was heavily influenced by the team’s work and is now in place at all VA facilities, thus collectively impacting care for millions of Veterans. The policy instituted new standards that actionable test results be communicated to patients within 7 days and those not necessitating an action within 14 days. Based on this policy and the team’s work, VA developed new performance indicators of timely communication of test results along with quality measurement guidance for data collection through the External Peer Review Program (EPRP).
Additionally, this team’s research informed the national CPRS View Alert Optimization Program to reduce low-value view alerts by:
On March 8, 2017, the Deputy Under Secretary for Health for Operations and Management disseminated the CPRS View Alert Optimization Program to all VA Network Directors. From March – June 2017, VAMCs implemented the program. On program analysis across 148 VA facilities, the median number of mandatory notification types at each facility decreased significantly from 15 to 10 pre- to post-intervention, respectively. Similarly, the mean number of daily notifications per PCP decreased significantly from 128 to 116. This national quality improvement program potentially saved 1.5 hours per week per PCP to enable higher value work.
This research has established HSR&D as a leader in the field of patient safety and diagnostic error reduction, informing several national and international patient safety initiatives and policy reports, including those by the National Academy of Medicine, US Department of Health and Human Services, American Medical Association, Agency for Healthcare Research and Quality, the CDC, and the World Health Organization.
Dr. Singh’s team uses an eight-dimensional sociotechnical approach to improve patient safety (more at www.bcm.edu/saferdx )
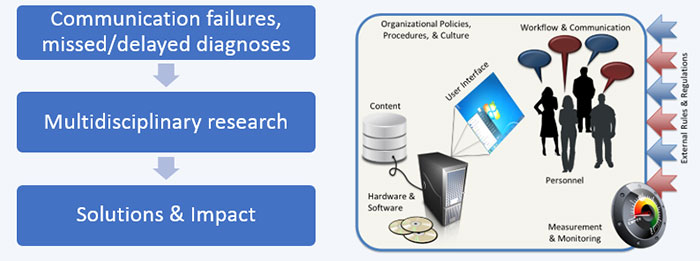
Hardware & Software – Developed decision support ‘AWARE: The Alert Watch and Response Engine’ – Developing Software to “Track and Catch” Missed Follow-up of Abnormal Test Results in a Complex Sociotechnical Environment. Smith MW, Singh H, et al. Appl Clin Inform. Jul 2013
Content – Developed a Checklist to improve CPRS ‘View Alert’ Notifications that informed the View Alert Optimization Project that saved VA providers 1.5 hours per week. Impact of a National QI Program on Reducing Electronic Health Record Notifications to Clinicians. Shah T, Singh H, et al. BMJ Qual Saf. Mar 2018
User Interface – Research informed better graphing of lab-test results in EHRs. Graphical Display of Diagnostic Test Results in Electronic Health Records: A Comparison of 8 Systems. Sittig DF, Singh H, et al. JAMIA. Mar 2015
Personnel –Developed a Toolkit now used throughout VA “Ten Strategies Providers Can Use to Improve Management of ‘View Alert’ Notifications in CPRS”. Ten Strategies to Improve Management of Abnormal Test Result Alerts in the Electronic Health Record. Singh H, et al. J Patient Saf. Jun 2010
Organizational policies, procedures & culture – Co-developed SAFER (Safety Assurance Factors for EHR Resilience) Guides – hosted on https://www.healthit.gov/topic/safety/safer-guides The SAFER Guides: Empowering Organizations to Improve the Safety and Effectiveness of Electronic Health Records. Am J Manag Care. Sittig DF, Ash JS, Singh H. May 2014
Workflow & Communication – Co-developed Communication of Test Results Toolkit (CTRT). Hosted on VA SharePoint Site http://vaww.vha.vaco.portal.va.gov/sites/DUSHOM/10NC/10NC3/CTR/default.aspx 2012
Measurement & Monitoring – Developed EHR-based triggers to flag patient records lacking follow-up of abnormal clinical findings suspicious for cancer. Electronic Health Record-Based Triggers to Detect Potential Delays in Cancer Diagnosis. Murphy D, Singh H, et al. BMJ Qual Saf. Jul 2013
External rules & regulations – Co-developed national VA policy regarding communication of test results to providers and patients - Communicating Test Results to Providers and Patients, VHA DIRECTIVE 1088. Oct 2015